Anodyne - Speed up collection of patient balances with electronic Patient Statements and Reminders

How the numbers tell you a grim story about patient balances?
Collecting patient balances is a long-term challenge for healthcare entities. A majority of medical facilities recover only a small proportion of what patients owe.
In its survey of 100 healthcare executives, Sage Growth Partners found that 36 per cent of the participants faced more than $10 million in bad debts. To make matters worse,6 per cent reported bad debts of over $50 million. On the recovery front, only half of these executives said their healthcare entities would realize more than 10 per cent of the outstanding patient balances. Furthermore, only 9 per cent stated they could recover more than 20 per cent of their dues.
Likewise, a study by TransUnion showed patient balances surging over 52 per cent between 2012 and 2017. So, patient balances are not only high but continue to increase at a worrying rate.
Patient balances are not just a problem for hospitals or Medical Centers. According to an authoritative Ipsos/Amino survey, 37 per cent of Americans say they would be in debt if they receive a medical bill of $100 or more. Besides, less than a fourth of Americans said they could repay a medical bill of over $2,000.
Against these challenges, consider the physician-patient relationship. It is a relationship of trust. The nature of this relationship makes recovering patient balances both delicate and challenging. So how do healthcare entities customarily address this problem? They instruct their administrative personnel to call up patients to collect their dues.
Nonetheless, collection phone calls can sound confrontational. For this reason, phone follow-ups are stressful for all involved. In the bargain, stress makes the already doughty task of providing care even more difficult to perform.
A convenient option to delegate your patient-balance collections is hiring third-party debt-recovery agencies. In the Sage survey, 36 per cent of the participants confirmed using third parties. Recovery agencies, though, often use a heavy-handed approach when collecting patient dues. Unfortunately, aggressive recovery methods do not promote a good hospital-patient relationship and often turn out to be counterproductive.
Why is a conventional collection approach not always effective?
The following steps represent how healthcare entities typically collect outstanding balances from their patients.
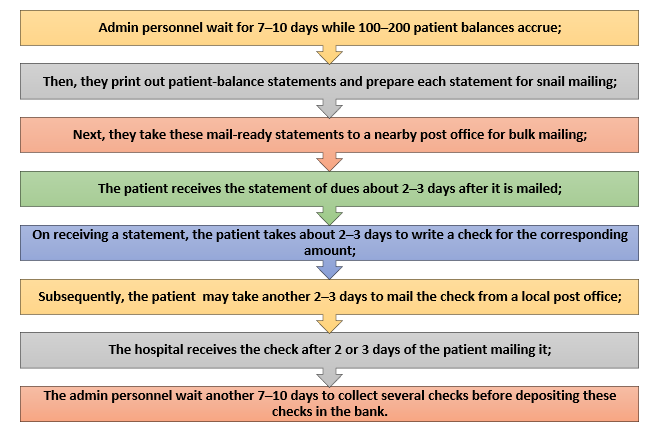
If all goes well, collecting the balance due from a patient can take between 22 and 40 days. Hospital employees can lose track of unresponsive patients during these long collection cycles.
Besides, your hospital may give up on small dues owing to the sheer effort and lengthy waits involved. As you have seen earlier in this whitepaper,small dues add up to big liabilities.
How Anodyne is a win-win, flexible payment method for both healthcare entities and patients
What is Anodyne? It is an easy-to-use, powerful patient engagement platform.
Anodyne offers the following benefits that can minimize your financial liabilities while drastically reducing the time and effort required to collect patient balance payments. It is environmentally friendly, too.

Your hospital’s liabilities can grow exponentially over time
Statistics provided earlier in this whitepaper show you how patient balances grow with time. One of the main reasons for poor collection rates is unclear patient statements.
Anodyne offers you a list of standard, easy-to-read e-statement formats. What’s more? We can customize these e-statements for your hospital. Clear patient-balance statements drive up recovery rates and reduce your financial liabilities.
Besides, technology implemented well is a force multiplier in revenue cycle management (RCM). Nonetheless, many admin employees at most healthcare entities are technology averse. The reason for this dislike is the steep learning curve involved with most RCM products.
Anodyne’s simple, straightforward user interface makes it easy to master and use. With Anodyne, you remove another obstacle to efficient and timely recoveries—complicated technology.
At Anodyne, we first carry out an exhaustive, customized product set up to address your specific needs. Your admin staff can then use this configured product with minimal training.
How to take the drudgery out of recovery work with Anodyne?
You saw how a traditional collection method is lengthy and cumbersome. Lost patient dues owing to long delays is another disadvantage of this approach.
Anodyne makes bill generation, emailing, and balance collections simple and quick. Simply put, it takes the drudgery out of printing, snail mailing, check collection, bank work, and messy phone calls.
So, how does Anodyne make life easier for you and your admin staff?
- Simple data entry through standard or customized billing formats creates Patient e-statements.
- Eliminates mundane effort involved in preparing paper Patient statements.
- No more awkward paper feeds, cartridge changes, postal procedures, and misprints.
- The product bulk emails e-statements to your patients’ respective email addresses.
- Cuts stationery-,postage-, as well as conveyance-related costs and efforts.
- Minimizes paperwork and bank visits associated with check deposits.
- Online patient payment option through a simple link in the email.
- Most payments are credited almost instantaneously to your hospital’s bank account.
The benefits you will enjoy when using Anodyne don’t just end here. Anodyne is built on the well-known, well-supported Salesforce platform. Based on this platform, you can conduct campaigns to engage your patients.
Campaigns generate timely and friendly reminders. For instance,you can send a politely worded reminder to each of your patients regarding their dues. This way, you prevent “bill not received” excuses. You can also run a campaign of automated text reminders to patients about their appointments to ensure prompt patient care. Reminders can be sent via text, IVR and/or emails. These reminders have twin benefits. The first is increased recovery rates through the online patient bill pay option; the second, trust-based doctor-patient relationships.
Besides, healthcare entities can minimize the involvement of ham-handed third-party recovery agents.
You can remove other impediments to patient-balance collections through Anodyne
Earlier in this whitepaper, you saw how higher patient balances adversely affect collections. Anodyne can address this issue.
You can work out a repayment plan for patients who owe large patient balances. Repayment plans offer payment through manageable instalments. Such plans make it easy for your patients to pay their dues over an agreed-upon period.
Another simple and handy option is that Anodyne can be set up for offline payments. While patients can read their e-statements online, they have the option to pay on their next hospital visit. Patients who are wary of online patient payment transactions find this option useful.
The third additional impediment Anodyne deals with is patient involvement. To use Anodyne and receive e-statements via email, the patient must sign a simple one-page agreement. This agreement ensures patient consent to receive electronic statements via email.
For your peace of mind, Anodyne is secure and safe to use
When faxing or mailing printed paper statements, the probability of a privacy breach is high. For example, the printed statement could be faxed to the wrong number. Alternatively, a postal envelope could open due to faulty sealing, revealing the patient statement.
Anodyne is a proven, simple-to-use technology. Many providers and patients have used it reliably for over two years. It employs authentication at every step in the billing-payment transaction.
The PDF e-statements generated through Anodyne are password protected and HIPAA compliant. Besides, a secure payment gateway from a reputed US bank ensures security of the online patient bill pay transaction.
Furthermore, Anodyne does not store your patients’ financial information when they pay online. This feature offers them total privacy.
Anodyne’s offline payment option, described earlier, gives your patients the flexibility to pay through credit or debit cards, cash, or check at the hospital. This way, your patients experience flexibility through a payment option of their choice.
Anodyne contributes in another significant way to your peace of mind. It is environmentally friendly. Your healthcare entity gets to eliminate large volumes of ink and paper by signing up for Anodyne. Visits to the bank and post office are also minimal. By adopting Anodyne, you contribute in a big way towards sustainability.
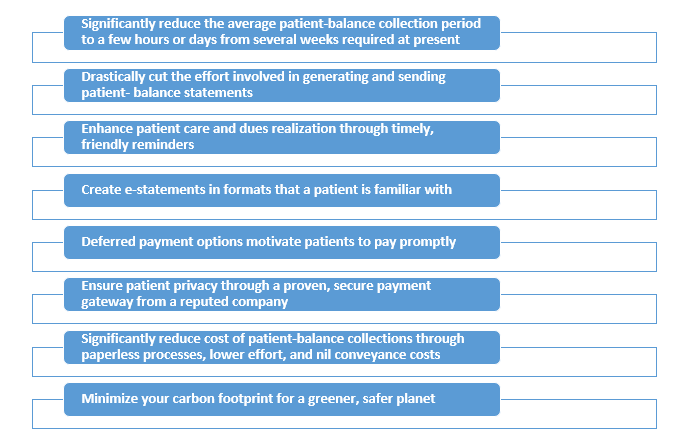
To summarize, Anodyne gives you the following advantages over traditional collection methods.

Reach out to us today for a no-obligation, quick evaluation of Anodyne. The little time you invest in evaluating this service will save many person-hours of effort and thousands of dollars for you.





































.png)











